India’s deadly second wave of coronavirus has left millions of its population infected and has placed extreme stress on the nation’s crumbling healthcare system. At its peak on 8th May 2021, India recorded more than 400,000 cases in a single day, accounting for over half the world’s daily cases and setting a global record that no country wants. According to experts, the actual figures are likely much higher than the official figures. The country was supposedly doing well up until February 2021. However, the recent spike has left the sick stranded and fighting for access to oxygen and medical supplies.
While much of the talk surrounding the dire crisis refers to the national level, ACI research goes one step further to explore the crisis at the state-level. They use the COVID-19 resilience index scores calculated using the Bloomberg methodology as a basis and make a comparison with ACI’s competitiveness ranking of India’s sub-national economies. The study finds that the more competitive sub-national economies are among the less resilient.
For example, more competitive economies such as Delhi and Maharashtra faced the largest burden of the second wave with high infection rates and fatalities. On the other hand, less competitive states in the North-eastern region such as Arunachal Pradesh and Assam have remained largely resilient to the COVID-19 second wave. The case of Kerala is worth highlighting, as it is one of the few states that is among the most competitive and most resilient. This is due to its history of proactive crisis management and robust healthcare system.
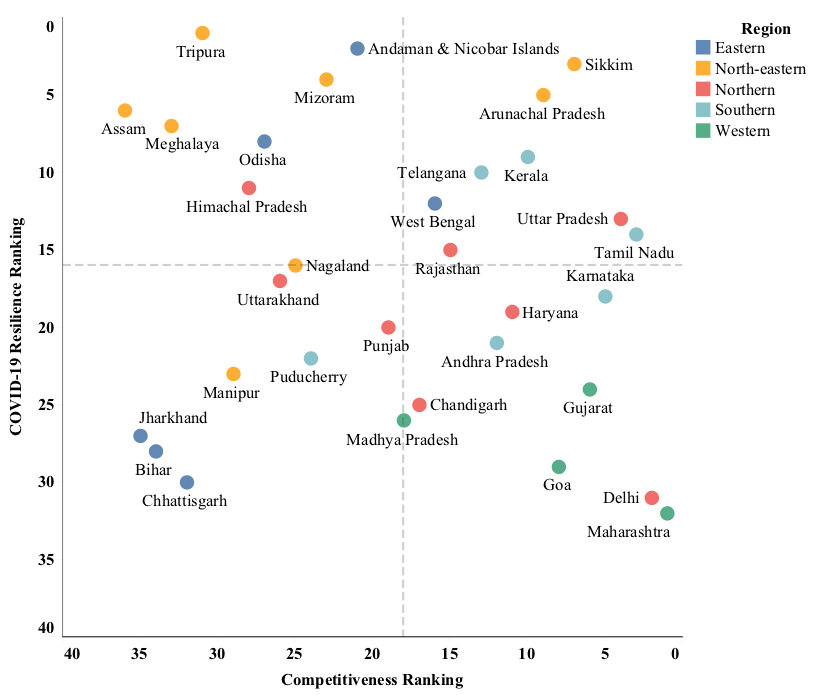
The states with better performance in terms of standard of living, showed higher resilience to the second COVID-19 wave. This is because they have a favourable ageing profile, old age dependency ratio and better healthcare infrastructure. The top competitive states have larger proportions of their population over 60 years old, and additionally lack adequate healthcare infrastructure to serve their more densely populated cities. As such, in April 2021 the country’s hospitals started running out of oxygen, hospital beds, and requisite drugs, with the national capital, Delhi, having less than 100 critical care beds at one point in time. The crisis exposed India’s meagre spending on healthcare, which has been around 3.6% of GDP for the past six years.
There are many crucial policy implications that come out of such research. Likely, the more competitive states could have weathered the second wave had they addressed the inadequacies in their public healthcare infrastructure and inequalities amongst their standard of living prior to the pandemic. Despite being the world’s leading producer of vaccines, less than 10% of India’s population has been vaccinated, as India was focused on competing with China to be a leading global player in exporting medical supplies rather its internal vaccination program. The new B.1.617 variant has further fuelled the spread, propelled by mass social gatherings, religious events, and election rallies with negligible social distancing. These events could have been deterred with responsible prioritisation and policymaking. Going forward, India’s policymakers need to take into serious consideration a science-based approach and suggestions from experts that include imposing a nation-wide lockdown, expediting vaccination, and constructing makeshift hospitals.
By Sunena GUPTA
Researchers: Ammu GEORGE, Sumedha GUPTA
